Extending Care Beyond the ER: How AI Voicebots Revolutionize Post-Discharge Patient Safety and Prevent Readmissions
While a smooth and successful surgery or an efficient treatment process in the emergency room may be half the battle, it is the beginning of the journey for the hospital. While hospital management may pay particular attention to patient care within the hospital walls, measuring their success rate by how many surgeries have been completed flawlessly, the real measure of success begins the very instant the patient leaves the hospital.
The most costly expense in the healthcare industry around the world is avoidable hospital re-admissions.
Consider this case study: An individual undergoes a complicated heart bypass procedure. He stays in the ICU and ward rooms under twenty-four-hour care by a group of committed nurses and doctors. Eventually, he is pronounced well enough to be discharged. However, before he leaves, he is provided with a bulky envelope filled with five sheets of discharge notes, nutrition guidelines, and a complicated chart of six medicines. He returns home.
Three days into his recovery period, he gets slightly confused regarding his medicine intake and inadvertently misses one dosage of his blood thinner medicine. He starts developing a fever with a bit of inflammation near his incision line, which he disregards thinking that it is merely a regular phase of his healing process. By the sixth day, this minor infection has transformed into an advanced stage of sepsis. Consequently, he falls unconscious, emergency medical assistance is summoned, and he is taken back into the ICU section of the hospital.
The vicious cycle of events is extremely harmful to the well-being of the patient, both physically and psychologically. Administratively, such an occurrence is extremely costly to the hospital’s efficiency. Additionally, in today’s healthcare system, which regulates hospital operations and insurance plans (CMS Hospital Readmissions Reduction Program in the United States, among others), hospitals incur massive losses due to frequent readmissions within 30 days.
The hospital wants to keep track of its patients when they go back home, but doing this manually is virtually impossible.
The Post-Care Communication Gap
A discharge patient is most likely in an extremely vulnerable position. The rush of adrenaline has subsided, and the patient is probably in pain and sleepy due to medication taken during the procedure. The patient nods in response to the explanations given by the nurse who is discharging them, but the moment they step out of the clinical setting, confusion strikes them.
In order to fill the hazardous void that exists between the patient’s hospital bed and their home life, the healthcare facility requires a dependable solution for daily patient monitoring. But using the most skilled, yet costly, professional nurses as call center personnel would be one of the worst possible wastes of medical talent available.
The nursing industry across the globe currently experiences a severe nursing shortage crisis. Nurses are required to remain at the bedside where they can monitor the patients’ vitals, manage the administration of intravenous therapy, and offer empathic care to their sick patients. What nurses aren’t expected to do is sit at their desks making calls to patients’ landlines day after day. It’s impossible for nurses to manually monitor high-risk individuals once they’ve been released from the hospital.
The AI Safety Net: Proactive Automated Follow-Ups

The visionary CMOs and Hospital Administrators are reinventing patient aftercare after discharge through the implementation of Conversational AI Voicebots provided by enterprise companies such as Archiz Solutions.
These systems do not replace the nurse at all; instead, they work as an endlessly scalable and non-stop safety net for the patients recuperating at their homes. In doing so, the technology automates the process of checking up on patients and separates the healthy ones from the at-risk ones who require human assistance.
An elaborated discussion about the automated workflow of the aftercare system follows:
Automatic EMR Integration and Daily Check-Ins: The hospital’s EMR system automatically activates the AI Voicebot. Depending on the particular discharge criteria being followed (e.g., orthopedic surgery discharge vs. maternity discharge), the AI is set up to call the patient every morning for seven to fourteen days after the discharge.
Clinical Symptoms Detection: When the patient picks up the phone, the AI talks with the patient using a soothing, gentle, and very empathetic tone. It can even speak in regional dialects to facilitate better communication. The AI asks specific, pre-programmed clinical questions about the health and well-being of the patient:
“Good morning, Mrs. Gupta. I am calling from the City Hospital’s cardiac care unit. I am checking on your recovery progress. Are you having any fever, chills, or breathing difficulties today? On a scale of one to ten, how severe is the chest pain? Have you taken your antibiotics in the morning today?”
Next Generation Sentiment Analysis and Triage of Critical Cases: The machine uses an advanced algorithm for analyzing Natural Language Processing (NLP) to understand the patient’s answers. For example, if a patient responds that he/she feels well, experiences only some minor discomfort rated on a scale of two points, and took his/her medications, the machine respectfully ends the conversation and automatically records this healthy information into the EMR.
But if the patient mentions some alarming symptoms like “my pain level is a 9 on the scale of 10, I am experiencing severe dizziness, and the wound area feels hot to the touch,” the machine understands the severity of the case and takes immediate action, even though it can’t provide any recommendations.
“Code Red” Protocol: At the very first sign of some critical symptom mentioned by the patient, the system ignores any existing protocol and automatically alerts the triage nurse who will receive the full text and audio version of the communication via her dashboard or cell phone application.
Now the nurse has actionable intelligence. They have the ability to contact the patient within three minutes in order to act, give advice or send for an ambulance if needed.
The Life-Saving ROI of Proactive Automation
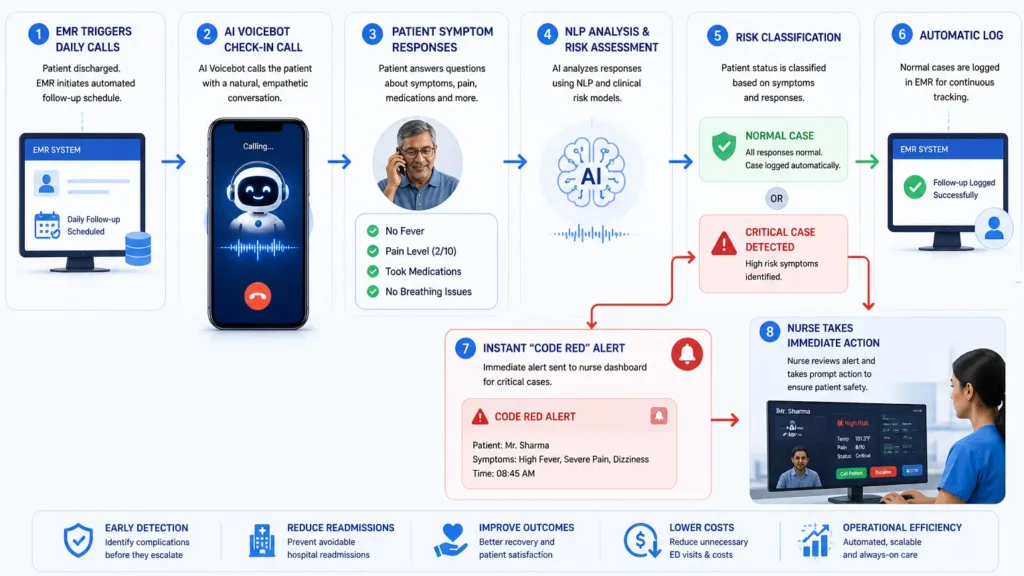
The ability to automate the follow-up process means that hospitals can monitor patients continually in ways never before possible. It provides benefits both clinically and financially:
Early Identification of Complications: Patients’ complications that occur after discharge (such as infections, blood clots, or adverse reactions to medications) can be identified early enough to allow for treatment of what could otherwise lead to an emergency situation.
Preventing Re-admissions: By taking immediate action, through phone calls or scheduling an outpatient appointment, you are able to ensure that the patient does not develop such serious conditions requiring hospitalization in a costly ICU setting. This results in significant savings in regulatory fines for the hospital.
Improving the Patient Experience: You make your patients feel truly cared about. Hospitals do not abandon patients after payment; rather, they continue to check on patients daily, which helps build patient loyalty and increases HCAHPS scores.
Giving Empowerment to the Medical Staff: The nurses don’t have to suffer anymore from the task of repeatedly making calls. They only call upon their clinical experience and intervene in cases where it really is necessary to save someone’s life.
The AI voicebot doesn’t substitute for the compassionate touch of a physician or a nurse but serves as a highly accurate and highly reliable radar which shows exactly which patient requires their compassion.

